Kathriona Devereux: Vaccination can be our saviour - with an injection of urgency
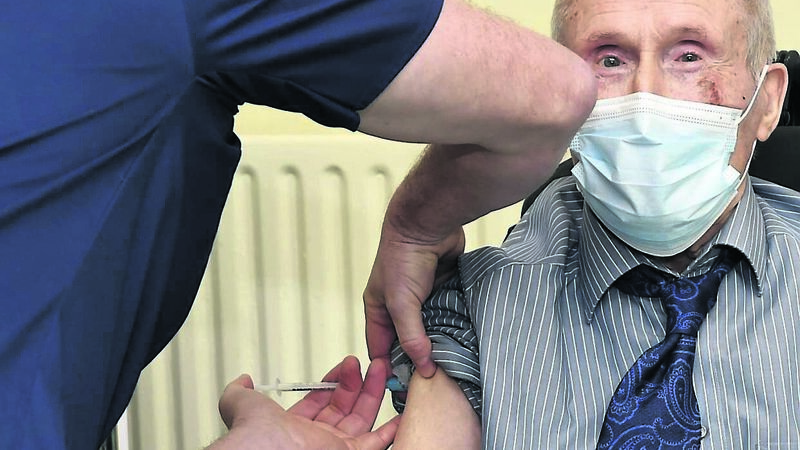
Twitter is full of selfies of hospital staff proudly receiving their dose and friends of mine said it gave them a big hopeful boost as they head into a nail-biting few weeks when the healthcare system and workers will be stretched to the max coping with the spike in Covid-19 cases.
It is only right that the people who put themselves in the firing line treating this virus are the people to receive the immunological armoury to protect them from infection. But I can’t wait for my appointment for vaccination and I particularly can’t wait till my granny gets hers.
When I recently heard there were Covid cases within her, previously untouched, residential home, my heart dropped. She is due to receive her vaccination on January 15 and I hope the wave of infection can be kept at bay long enough for her to receive the vaccine and the hope of some kind of normal life.
Residents of long-term care facilities are at greatest risk of severe illness and death. In Ireland, in the first wave of Covid-19, 56% of deaths occurred in this setting and more than 30% of cases were in healthcare workers. Vaccinating those two groups is a clear priority, but who gets jabbed next?
A friend of mine contacted the GP of her 87-year old-mother, enquiring about future vaccination timelines and was told the GP practice had no information about when or how vaccination will happen.
The 87-year-old living in the highly infected county of Monaghan will keep cocooning and praying and hoping her vaccination will come before she contracts the virus.
According to Ireland’s Covid-19 Vaccine Implementation Plan, adults aged 70 and older will be next in line. Starting with the oldest and working down. Good news for the Monaghan granny, even though the timing and location of when this will happen is yet to be determined.
The plan identifies 15 population groups and ranks them according to priority and provides the rationale behind the ranking. Adults aged 18-64 with chronic medical conditions such as heart, respiratory, liver and kidney disease as well as diabetes, obesity and immunosuppression due to disease or treatment are seventh in line to be vaccinated.
Adults living or working in crowded accommodation where self-isolation and social distancing is difficult to maintain are high are ninth.
“Those who are essential to education and who face disease exposure — primary and second level school staff, special needs assistants, childcare workers, maintenance workers, school bus drivers etc,” are 11th on the list.
That these vaccines require ultra cold storage is one factor, as is supply of vaccine from manufacturers, availability of workforce, provision of technology to administer and monitor the roll-out, and the huge communications effort required to inform the public about the vaccines and assure them of their safety.
Asking questions about vaccines is a good thing, getting answers from unqualified, non-medical personnel on a Facebook group or Twitter echo chamber, instead of the dedicated immunisation experts, is not.
This mass vaccination effort is being replicated around the world. Israel has stormed ahead of lackadaisical countries, with more than 10% of the population already vaccinated. Securing big vaccine supplies early and 300 vaccination centres working 24-7 have made a big impact.
Israel is still in the midst of a third strict lockdown but is hoping to have a huge proportion of the population vaccinated by March, with a resumption of some kind of normal life soon after.
With concerted and dedicated effort, the course of history can be changed. In New York in 1947, a case of smallpox imported by a businessman returning from Mexico sparked a small outbreak that spurred city health commissioner Dr Israel Weinstein to vaccinate the whole city. Volunteer vaccinators, as well as health care professionals, gave as many as eight doses a minute and vaccinated five million New Yorkers in two weeks. The smallpox outbreak was snuffed out with 12 infections and two deaths.
Without decisive and quick action, the alternative history of New York City could be profoundly different.
It’s unfair to compare post-war America with 21st century Ireland but a speedy and dogged roll-out of the Covid-19 vaccination will save lots of lives and lots of money. We can’t afford to be leisurely about it.
Living a life free of the fear of contagious diseases like polio, TB and cholera. The multitude consequences of a rampant infectious disease have been laid bare the past year.
However, for all the success of vaccines, which save up to two million lives every single year, smallpox is the only infectious disease that has been officially eradicated.
Humans will be living with Covid-19 for a long time to come but vaccination remains one of the most powerful tools we have at fighting it.
That is why a slow or faltering vaccination campaign is not an option. Real urgency is required.
For all its failings, the Irish healthcare system is bursting with able and competent people, the government should enable and support them to lead the vaccination effort so that this difficult January will be our last strict lockdown.







 App?
App?




