Cases of South African Covid-19 variant discovered in Ireland
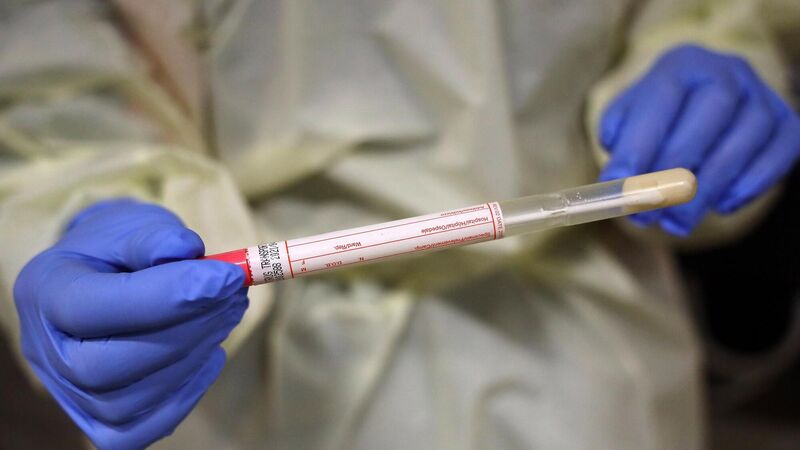
There are fears that the mutated form of coronavirus could be resistant to vaccines, although public health chiefs here say there is not enough information to determine that.
Three cases of the South African variant of Covid-19 have been discovered in Ireland, the chief medical officer has said.
There are fears that the mutated form of coronavirus could be resistant to vaccines, although public health chiefs here say there is not enough information to determine that.
The news came as a record daily total of 8,248 confirmed coronavirus cases were recorded in Ireland, along with 20 further deaths - the highest figure since May.
Chief medical officer Dr Tony Holohan said: "All of the cases identified are directly associated with recent travel from South Africa.
"Anyone who has travelled from South Africa recently is advised to self-isolate for 14 days and identify themselves through a GP for testing as soon as possible.
"We are particularly advising healthcare workers travelling from South Africa, that it is essential that they self-isolate for 14 days before entering/re-entering the workplace.
"While this variant has not yet been identified in many European countries, we believe the identification here reflects the extent of genome sequencing surveillance in Ireland."
Nphet's virology expert Dr Cillian De Gascun said: "There is currently not enough information available to determine whether this variant poses a possible risk related to vaccine match and effectiveness.
"The antigenic characterisation of this new variant is ongoing, and results are expected in the coming weeks."
He added: "The ECDC assessment states that preliminary analyses indicate that the South African variant is associated with a heightened viral load and may have increased transmissibility.
On Friday, Health Minister Stephen Donnelly has said staff and residents in nursing homes across the country will receive their first vaccines within 16 days.

He told RTÉ News: "What we had been doing was keeping one week of supply as a buffer, because there had been supply chain issues.
"Pfizer have been delivering solidly on time, what we're doing is we're taking 26,000 doses from the buffer that we were holding and accelerating, essentially doing three weeks worth of vaccinations in the next 16 days.
"Everyone in the nursing homes, the residents and the staff will have had their first dose, and we will move immediately then on to the second doses."
The Pfizer-BioNtech vaccine requires two doses, administered 21 days apart.
Ireland is set to receive an additional 3.3 million vaccines after the European Union reached a deal with Pfizer and BioNTech for 300 million more doses of their Covid-19 vaccine.
Meanwhile, health officials are preparing emergency plans across hospitals as they expect the number of Covid-19 patients to more than double over the coming weeks.
Hospital staff are bracing themselves for a surge in coronavirus patients as the number of cases escalate.
Anne O'Connor, HSE chief operations officer, said they are preparing for 2,500 coronavirus patients in hospital, with up to 400 people in ICU over the coming weeks.
There are currently 1,151 people in hospital with coronavirus and 101 patients in ICU.
Ireland's coronavirus reproduction number is now between 2.4 and 3, the highest level seen throughout the pandemic.
"We hope we don't get there and the action people take will impact on that," Dr O'Connor told RTÉ.
"Part of the challenge is time lag. When we hear the big numbers announced every day, in terms of the number who test positive, it takes a number of days or even a week for that to translate into hospital figures and another week again for ICU figures."
The senior HSE official said that all hospital sites have surge capacity and will scale up to respond to higher numbers.
It comes as Cork University Hospital (CUH) is preparing to trigger its emergency tiered escalation plan over the rising number of cases.
Dr O'Connor said they are "concerned" about a number of sites in Cork.
"We have scaled back on non-Covid work on much of our sites, we are prioritising Covid and there are risks in that both for people who haven't been able to access services and had appointments cancelled this week," she added.
The decision to suspend non-Covid treatments is to maximise capacity in hospitals to care for the sickest patients who have Covid-19, the HSE said.
Dr O'Connor also urged the public to use community assessments hubs across the country which are staffed by GPs, health professionals and nurses.
She said one of the major challenges is people turning up to emergency departments with Covid-19 without having contacted their GP first.
She added: "Covid is a very scary thing because it impacts on your breathing and people feel that they should go to hospital themselves, but we have to remember that GPs working around Ireland are senior clinicians and if they feel someone needs to be in an emergency department then they probably do."
Michelle Kingston, an emergency department nurse at CUH, said they are at crisis point.
"A lot of our staff are out sick with Covid or out because of contacts. That's the challenge for us," she said.
"We still have an influx of patients coming in and we have to deal with that."
More than 180 nurses at the hospital are not able to work because they either have the virus or were a close contact with a confirmed case.
Ms Kingston fears that there will be more staff out sick because of the levels of contact with confirmed cases.
"It's all hands on deck," she added.
"We are always protected in PPE but you are in close contact (with patients) and sometimes you still get it."
She said that a lot of people with Covid-19 are self-referring to the emergency department which is causing difficulties.









 App?
App?


