Our baby arrived 10 weeks early... a Cork mum shares her story
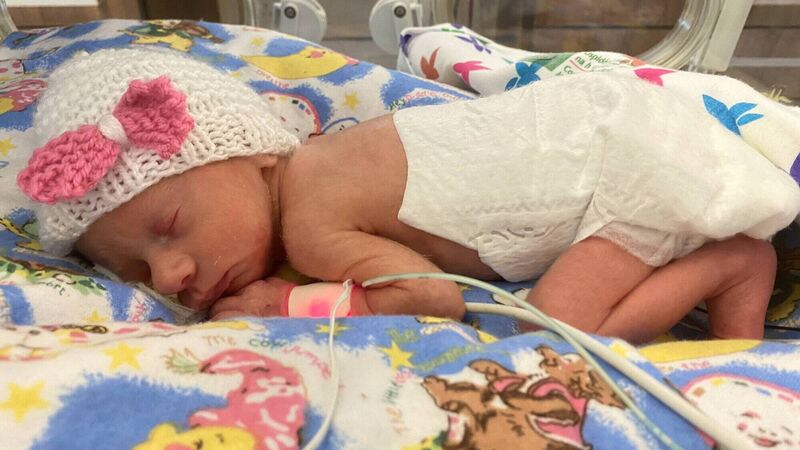
Amy Fogarty and John O'Connell's daughter Síofra, who was born 10 weeks early.
World Prematurity Day is marked every November 17. An estimated 15 million babies are born too early every year, which is one in 10.

Speaking just eight days after the birth, Amy, originally from Dublin, recalled the emotional rollercoaster herself and partner John O’Connell have been through since becoming parents.
The 34-year-old junior doctor, who specialises in obstetrics and gynaecology, had become concerned by her baby’s lack of movement and decided to get checked out. After being kept in hospital overnight, discharged for a day, and then undergoing subsequent tests including a trace on baby’s heart, it was decided that the baby was better out than in, and to deliver her.

That unexpected decision was made at 11am, and Siofra was born by C-section at 7.31pm.
Amy has performed her share of C-sections, but this was a whole new experience for her.
“It was a very surreal feeling. I don’t remember too much about the moments after she was born. She was wrapped in a turkey bag to keep warm and I remember she had dark hair and reaching out to touch her.”
After some pictures were taken, Síofra was swiftly taken to the neo-natal unit with John, and since then it’s been a series of ups and downs for the couple.
“There’s elation that she’s doing well, but lots of guilt too. You think that the only thing you had to do for them was to provide a safe place and you feel bad that, for whatever reason, that didn’t work out. I hope to get answers from my placenta, but I might never know what happened.

“I’ve a high stress job, and you wonder was that it; or was it the pandemic, or maybe just bad luck. I feel bad seeing what she’s going through when she should have been in my tummy for another 10 weeks,” said the new mum.
That first night in the hospital after giving birth, Amy remembers, was her worst. She had a spinal epidural so was unable to go the unit where at this point her little girl had been intubated to assist with breathing.
“There were a million thoughts going through my mind. I went down the next morning at 6am, and it’s all a bit of a blur. I’m not afraid of medical equipment, but her being in there was terrifying for me.”
Amy speaks highly of the nurses and all the staff in the 50-bed neo-natal unit.
“They really make you feel like you’re a normal parent and get you involved, encourage you to talk to the baby and show you tips and tricks.”

Síofra was three days old when Amy was able to pick her up: “It was mad really, she was so completely perfect with her eye- lashes, fingers, nails, all there, but just so tiny.”
She’s now doing really well and breathing on her own. Babies don’t learn to suck until 34 weeks so she’s being tube fed and Amy is expressing milk for her, and also availing of donated breast milk available at the hospital.
Being discharged from CUMH without her daughter was understandably difficult.
“It was really tough leaving but we knew it wasn’t a case of her being out in a week, so we had to get into a routine. In the hospital I was going down twice a night to express and feed her, and it was a vicious circle. That’s the best thing I can do for her now so I need to ensure I can do it.”

She honestly admits that her experience will make her see things differently as a doctor.
“As a doctor you make a choice to deliver a baby for whatever reason and you think of the there and then. This was a massive eye-opener for what a premature baby means to everyone involved, the whole family.”
Part of what that means for Amy is a grieving process for what she had anticipated her pregnancy would be like.

“I’m grieving the loss of a normal experience, the excitement of my bump growing, setting up the house. We lost all of that.”
Covid has also naturally impacted the neo-natal unit. It means that, unless a baby is very ill, only one parent can be there at a time. Right now the couple travel to the CUMH and take it in turns to be with their daughter.
“It works for us as we have a small baby, but a well one. We just have to grow her, which takes the pressure off. Having separate times gives dads a chance not to be standing in the background and also takes the pressure off the mum, who might feel she has to be there all the time. But if she was unwell, it would be a different kettle of fish entirely,” said Amy.
They also ring the unit nightly at 10pm and again at 4am.
“I’m up pumping so I call and it’s really reassuring to check in. The staff there do such a good job, and have made the most traumatic and difficult experience of my life bearable,” she said.

SUSAN Vaughan has been a nurse in the CUHM neo-natal unit for more than 10 years.
She has seen her fair share of happy and sad outcomes, but throughout it all her focus is to give individualised care to every baby in their care.
And Susan says that, regardless of their gestation, babies can communicate their needs once you know how to read their cues.
Susan, from Fermoy, puts a huge focus on premature babies’ developmental care and was one of the first nurses in the country specially trained to give a voice to the newborn.
“Lots will need nasty IVs to survive, and it’s important that their only touch isn’t one of pain, but something more positive. It’s about training the pathways of their brain to develop,” she said.
She encourages lots of skin to skin contact between baby and mum and dad, and says premature babies don’t like stroking (which feels like being tickled) but prefer the gentle laying of hands on their skin.
“But they’re all different, no matter what gestation they’re born, and they all get individualised care here.”
As premature babies senses aren’t fully developed (they can hear but not fully see), noise and light are kept to a minimum.
She sees her role not as mum to the babies, but as someone who helps parents to get to know their new born and gets them involved with nappies, baths and feeds.

“Most babies leave around their due date, but some have been here for six or seven months, and for others this has been their home so for those parents it’s about making memories.”
Challenges don’t always end on discharge either and lots of parents, she says, report Post Traumatic Stress Disorder after what they’ve been through.
“Adrenaline keeps them going in hospital but the trauma of what they’ve been through can often hit when they get home,” she said.
The family-centred unit is staffed by 13 neo-natal nurses, and a multi-disciplinary team comprising an occupational therapist, speech and language therapist (to help with feeding), and dietician, among others.
Understandably, Covid has impacted how they operate. Back in March, and for nine weeks, only mothers were allowed to be with their babies.
“Dads were only allowed in extreme cases, which was just heart-breaking. They’re both allowed in now, but not together.”
An annual coffee morning to mark World Prematurity Day organised by Susan for over 10 years has also been a victim of the pandemic. The morning saw parents, both past and present, come together and remember the challenging journeys that babies and families undertake due to prematurity. It was also a great opportunity for staff to meet the babies again and to see how they are doing, as well as it being a great opportunity for new parents to meet others in the same situation. Susan explained how the event usually takes place in Brú Columbanus, where many parents of babies in the unit would have stayed, and it’s a chance to say goodbye and thanks to staff there too.
Instead of the coffee morning, the unit is making a video for their social channel to capture their message of hope and love.
Susan is a mum of two girls, aged 22 and 20: “It really does go by in a heartbeat but I get my cuddle fix in the unit; and I can identify with parents who hand their babies over to us and put so much trust in us.”
As intense as it is, Susan loves her job and says all their miracles make it so rewarding: “But working here teaches you not to sweat the small stuff. It really puts things into perspective.”







 App?
App?


